
Working in Health Promoting Ways
Working in Health Promoting Ways (WiHPW) is a resource for health and community workers to address the causes of ill health, reduce the burden of chronic conditions, and create a more sustainable health system.
The vision of wellness is that it nurtures, supports and sustains health via a holistic approach to emotional, financial, physical, social and spiritual factors.
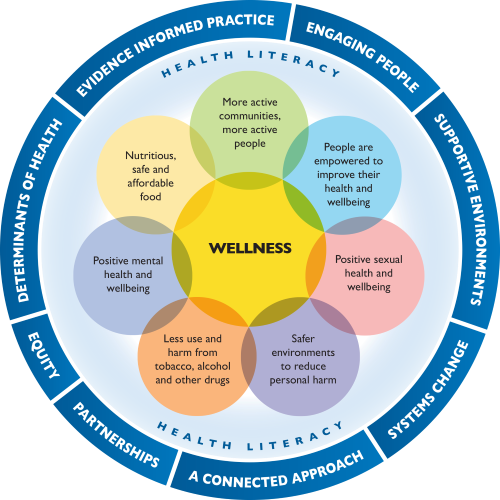
Principles of practice
WiHPW consists of eight principles of practice:
- evidence informed practice
- determinants of health
- equity
- partnerships
- a connected approach
- systems change
- supportive environments
- engaging people
Learn more about the principles of practice.
Health literacy
- Health literacy is how a person can find, understand, make decisions, and act on health information. How health and community organisations are set up and communicated make it easier to access health information.
- Learn more about health literacy.
Priority areas
There are seven identified priority areas for health promotion action:
- more active communities, more active people
- nutritious, safe and affordable food
- positive mental health and wellbeing
- less use and harm from tobacco, alcohol and other drugs
- safer environments to reduce personal harm
- positive sexual health and wellbeing
- people are empowered to improve their health and wellbeing
Learn more about the priority areas.
Planning resources
Access our Health Promotion and Planning Resources
Training opportunities
Discover current training opportunities for Working in Health Promoting Ways.
Contact us
For more information about Working in Health Promoting Ways email [email protected].
Inspiring Stories

LGBTIQ+ inclusive healthcare learning resources

Transition to high school, dealing with change program

Weavers - support along the dementia caring journey

